Safeguard
Operating a safe, reliable blood system
Canadians count on us to provide a secure supply of high-quality blood and blood products.
Our donor centres, supported by recruitment initiatives that encourage Canadians to donate blood, are the critical “front end” of our blood supply chain. Our team members at these centres collect the red blood cells, platelets and plasma that hospitals and clinics need to treat patients.
Red blood cells
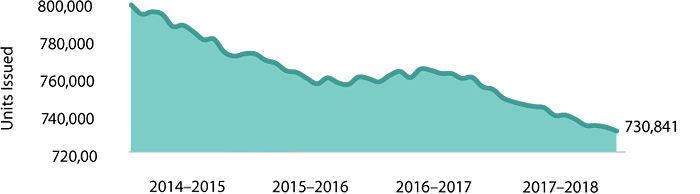
In 2017–2018, Canadian Blood Services shipped 730,841 red blood cell units to hospitals. This figure represents a customer order fill rate of over 99 per cent, meeting customer needs without compromising patient care.
Demand for many blood products has fluctuated in recent years, which makes forecasting a challenge. Hospital orders for red blood cells have been falling steadily, declining by five per cent since 2014–2015, though we expect this trend to taper off in the future.
Shipments of red blood cells
At the same time, our continued focus on supply chain management over the past few years has led to fewer discards of whole blood and red blood cell units. This past year we saw the fourth consecutive drop in the annual discard rate, which for the first time fell below six per cent (5.8%). The number of outdated units also fell to an eight-year low of 0.1 per cent.
Having fewer discards enables us to meet hospital demand with thousands fewer whole blood collections each year. In addition to reducing waste, these improvements have saved or avoided millions of dollars in costs. We will continue to focus on improving the discard rate, generating further savings in the future.
Platelets
Platelets are the small, disc-shaped cell fragments in whole blood that help to form clots that stop wounds from bleeding. When patients don’t have enough platelets as the result of disease, drug treatments, trauma or surgery, this can compromise the clotting process and be life-threatening.
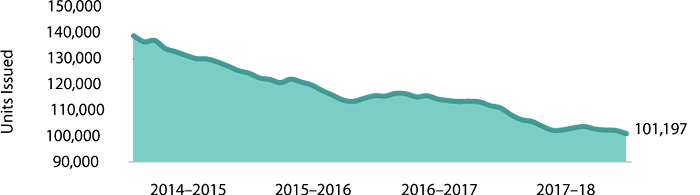
In 2017–2018, we shipped 117,063 units of platelets to hospitals, down from 119,974 units in the previous year. Most of the platelets we supply to hospitals come from whole blood donations. We also collect platelets through apheresis, a process that mechanically separates one component of collected blood while recirculating the rest back to the donor. Although apheresis helps us to more precisely match platelets to specific patient needs, it’s also more costly than deriving them from the pooled donations of many donors.
Shipments of platelets
During the past year, we decided to manufacture more platelet doses from pooled donations of whole blood rather than through apheresis collection as we have done previously. In doing so, we took into account the needs of sensitized transplant patients whose blood carries antibodies that attack foreign tissue, as these patients tend to fare better with platelets collected via apheresis. While ensuring the needs of these patients were met, we were still able to reduce the number of platelet donations needed overall, which saved health systems about $1 million. We were also able to gain even better cost-efficiencies with a new method that safely extends the shelf life of platelets from five to seven days, provides more precise bacterial testing and reduces waste by 40 per cent.
For now, platelets will continue to be widely used in cardiac and cancer care. Looking further ahead, we expect that new approaches to patient blood management, as well as medical innovations such as chemotherapy agents that are less toxic to bone marrow, could reduce the need for platelet transfusions.
Plasma
Plasma is the protein-rich liquid in blood that helps other blood components circulate throughout the body. Some of the plasma we collect is used by hospitals to treat trauma and severe bleeding. We collect plasma either by separating it from whole blood after a whole blood donation or by collecting it on its own through apheresis.
Plasma is used both for transfusions and for fractionation into a range of specialized proteins for therapeutic use.
In 2017–2018, we shipped 30,374 litres of plasma for transfusion to hospitals (101,197 components issued), down from 32,445 litres (111,141 components issued) in the previous year.
Shipments of plasma for transfusion
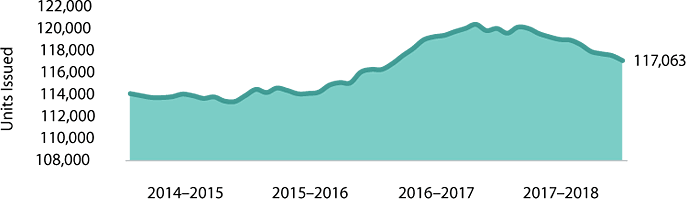
Demand for plasma for transfusion has gone down by 25 per cent since 2014–2015. This decline is the result of changes in transfusion practice and the increased use of alternatives to plasma for transfusion, like prothrombin complex concentrates and, to a lesser extent, solvent detergent plasma.
Most of the plasma we collect is used to make plasma protein products (PPPs). One of the most critical products is immune globulin (Ig), which is used to treat immunodeficiency disorders, autoimmune disorders, hematological disorders and neurological disorders.
Other PPPs include albumin, often prescribed for burns and trauma, as well as clotting factors for some bleeding disorders. (Some of the clotting factors we carry are made from plasma; others are synthesized from recombinant DNA.)
Products made from plasma are created through a process called fractionation. We ship plasma to contract suppliers in the U.S. and Europe, which manufacture products that are then shipped back for use by patients in this country.
In 2017–2018, we shipped 171,564 litres of plasma for fractionation into PPPs, down from 174,700 litres in the previous year.
Canadian plasma shipments for fractionation by source
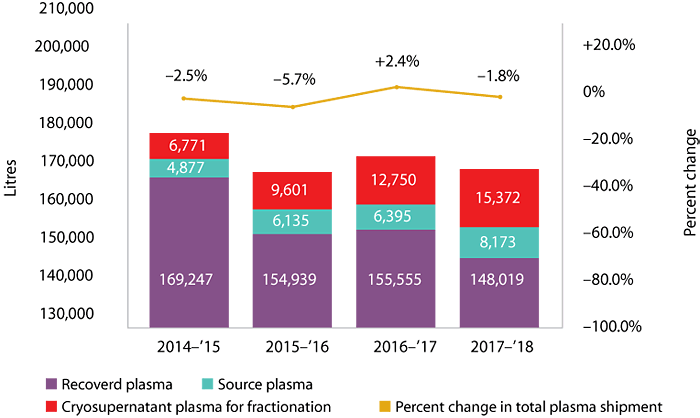
We also buy some plasma-derived products and recombinant products from manufacturers abroad that meet the stringent safety and quality standards of regulators such as Health Canada and the U.S. Food and Drug Administration.
As worldwide demand for PPPs continues to grow, ensuring there’s enough plasma to manufacture into Ig for Canadian patients is a key priority. Over the next several years, we plan to collect significantly more plasma to increase Canada’s plasma sufficiency for Ig.



